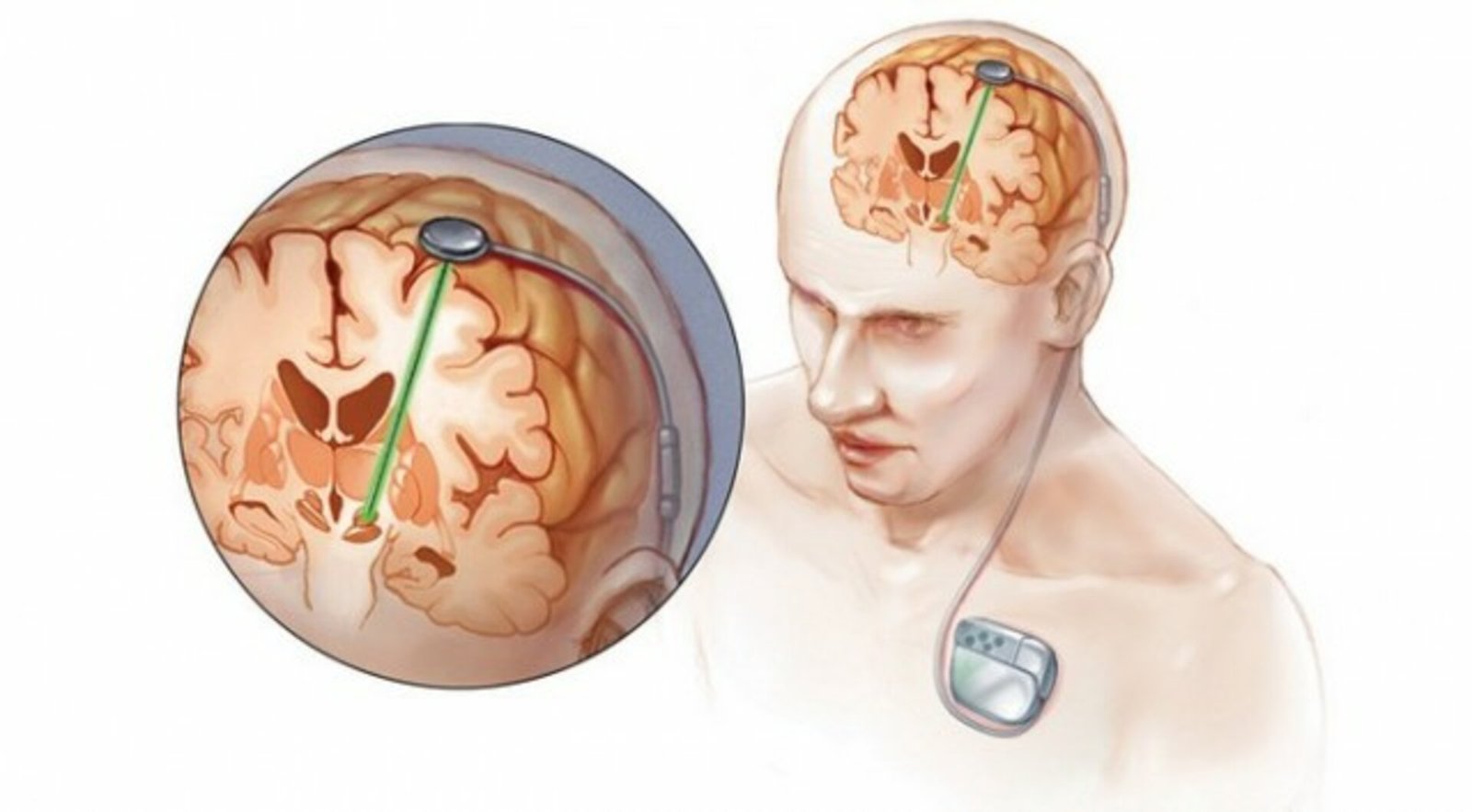
Deep Brain Stimulation
Deep brain stimulation (DBS) comprises the implantation of a device called as neurostimulator which sends electrical impulses, to precise targets in the brain (brain nuclei), through implanted electrodes.
The DBS system consists of very thin DBS Lead which contains four- eight electrode contacts which are implanted into the target area in the brain. The lead extends through a burr hole in the skull and is connected to the extension wire that is then connected to an impulse generator or pacemaker which is implanted under the skin over the chest. DBS exerts its therapeutic effect by delivering electrical impulses to the target region.
Deep Brain Stimulation is an alternative to ablative surgeries which were offered in the past for Parkinson’s disease and other related movement disorders. The common targets for DBS surgery within the brain, for movement disorder include, subthalamic nucleus (STN) for Parkinson’s disease, Ventrointermedius nucleus of thalamus for tremors, and pallidum for dystonia. Though each of this target sites can be used for different movement disorder, we believe that these are best for the respective disease as indicated.
During the last decade deep brain stimulation (DBS) has become a routine method for the treatment of advanced Parkinson’s disease (PD), leading to striking improvements in motor functions and quality of life of PD patients. It is associated with minimal morbidity. More than 1,50,000 patients must have undergone DBS surgery for Parkinson’s disease around the world.
The therapy of Deep Brain Stimulation requires additional expertise over conventional stereotactic techniques that are required for functional neurosurgical procedures for movement disorder. It needs cautious understanding of the principles of DBS, understanding of the disease being treated and merging the medical therapy along with stimulation to achieve smooth control of the disease. Jaslok Hospital & Research Centre has been able to develop a multi-disciplinary team to undertake this surgery.
The team comprises of Neurosurgeon, Neurologist, Clinical research fellow, Parkinson’s disease nurse, neuro-psychiatrist and physiotherapist. Expertise of speech therapist, occupational therapist and other specialists is obtained when required.
The success of the therapy largely depends on the selection of the appropriate candidate patients and on the precise implantation of the stimulation electrode, which necessitates careful imaging-based pre-targeting and extensive electro-physiological exploration of the target area.
How (DBS) Work
The brain cells function by electrically encoding, processing and transmitting information. Deep brain stimulation affects the electrical functions of neurons, but the mechanism by which it alters those functions, are unknown. According to some hypothesis, the reduction of the effects of an abnormal neuronal activity occurs because of inhibition, depolarization blockade or the adjustment of neuronal activity to a constant rate.
• Inhibition – The depolarization of axons terminating in target structure by deep brain stimulation causes these terminals to discharge and release neurotransmitters. Deep Brain Stimulation may cause a flood of inhibitory neurotransmitters that effectively shuts down neurons in the target structures.
• Depolarization blockade – If a neuron is constantly depolarized but below the threshold need to produce an action potential, the threshold for producing an action potential increases. Neurons firing are difficult as the threshold increases.
• Altering erratic neuronal activity – Deep Brain Stimulation alters the abnormal discharge activity that results from the disease. It has been suggested that irregular or chaotic firing of neurons may be more disruptive of normal function than a constant and regular pattern of activity. Deep Brain Stimulation drives the abnormally discharging neurons into a pattern of more regular firing that is less deleterious.
• Indications – Deep brain stimulation (DBS) has become an effective therapy option for several different neurologic and psychiatric conditions, including PD. It currently has the US Food and Drug Administration approval for Parkinson’s disease, essential tremor, dystonia and obsessive-compulsive disorder. For PD treatment, it is currently approved specifically for those patients suffering from complications of pharmacotherapy, including motor fluctuations or dyskinesia and a disease process of at least 4 years of duration. Studies have demonstrated DBS and medical management is superior to medical management alone in selected PD patients.
Deep brain stimulation (DBS) is done in patients with a variety of neurologic conditions such as:
• Essential tremor
• Parkinson’s disease
• Dystonia
• Epilepsy
• Tourette syndrome
• Chronic pain
• Obsessive compulsive disorder
• Major depression
Risks and Complications
DBS is overall considered a relatively safe neurosurgical procedure with low mortality. However, akin to other surgical procedures, DBS surgeries can be complicated by intraoperative and postoperative complications such as intracranial bleeding, seizure, stroke, hardware malfunction, infection, prolonged length of hospitalization, and postoperative confusion.
One of the common issues of DBS complication is the erosion or thinning of the skin over the implants. This occurs due to various reasons, ageing, superficial pocket, weight of the implant etc. Patient should maintain good hygiene and care of the implant sites, right from the scalp to the pacemaker site. One should also watch out for the extension wire connector site as it is another common area of erosion; this is located behind the ears.
Many times, patient develop stimulation related side effects. The most common being speech, and gait disturbances. Sometimes patient also develop paraesthesia and that is tingling and numbness in the areas of stimulation. This problem can be related to adjustments of this medication and others can be because of the stimulation induce side effects careful programming and understanding of this problem helps to minimise or eliminate most of them.
